
President and Chief Executive Officer
I recently had the opportunity to participate in a terrific conversation with two of my fellow CEOs on a Meeting on the Mesa panel from other leading gene therapy companies entitled “State of Play in the Vector Arms Race: Perspectives on the Future of Gene Delivery.”
From that title, you might have been expecting fireworks, with each of us defending one delivery mechanism as the future of gene therapy. In fact, it was quite a friendly conversation – and not just because we all happen to get along well. While we each are passionate about our chosen approach to gene therapy, we agreed that each modality has its unique strengths. What is most critical is matching the right modaility and vector to the right disease.
All gene therapies share a common goal: To deliver the genetic code patients require to begin expressing the specific active protein they need for healthy cellular function. Picking the most appropriate delivery mechanism to enable this process has important implications for the potential safety, efficacy and durability of the therapy for a specific medical indication and especially with respect to its treatable patient population.
I’ll leave it to my fellow panelists, Drs. Geoff McDonough of Generation Bio and Asa Abeliovich of Prevail Therapeutics, to share their perspectives on non-viral and in vivo AAV gene therapy, respectively. At AVROBIO, we work exclusively in ex vivo lentiviral gene therapy. Here’s why:
Proven record, broad utility
Lentiviral gene therapy has been used since the early 2000s to treat hundreds of patients in multiple trials – including four clinical trials of AVROBIO’s investigational gene therapies in lysosomal disorders.
We believe that lentiviral vectors have both a proven record and broad utility in lysosomal disorders. The proven record refers to the strong track record of safety and durability academia and industry have compiled over more than 12 years. The phrase “broad utility” covers two key points: the broad applicability across patient populations and the broad reach of the therapy to potentially address symptoms throughout the body and brain.
Let’s explore these statements a bit more.
Our process begins with the patient’s own hematopoietic stem cells, which are collected in a routine clinical process called apheresis. A lentiviral vector is used to insert a therapeutic gene into those stem cells in a manufacturing facility (hence, “ex vivo”), rather than in the body. Because our lentiviral vector does not enter the body, we don’t need to exclude patients with pre-existing antibodies to the vector – an issue that can limit the reach of, for instance, AAV-based gene therapies.
Lentiviral vectors are designed to integrate the therapeutic gene directly into the patient’s chromosomes. This means that when the original batch of genetically modified stem cells divide and proliferate into trillions of daughter cells, each of those progeny is expected to carry the therapeutic gene and be potentially capable of expressing the active protein the patient needs. This integration means that we do not need to flood the cells with lots of vector – a low number of therapeutic genes per cell may be enough to produce the required threshold of active protein, which is typically agreed to be 10-20 percent of normal values for an enzyme due to its catalytic nature. This approach is designed to be durable for years; it literally is in the patient’s DNA. If proven to be safe and effective, lentiviral gene therapies may therefore be appropriate to use as one-time treatments for any tissue or organ, such as the liver, that undertakes growth and/or regeneration.
Perhaps the advantage we’re most excited about is that lentiviral gene therapy, when combined with the personalized conditioning agent busulfan, potentially enables true “head-to-toe” treatment.
Potentially enabling true head-to-toe treatment
Before their genetically modified stem cells are infused back into them, lentiviral gene therapy patients must first undergo a brief personalized conditioning regimen to make space in the bone marrow for the treated cells to engraft. At AVROBIO, we use personalized conditioning deploying state-of-the-art precision dosing of the single conditioning agent busulfan, which is designed to maximize the chances of the treated stem cells engrafting in the patient’s bone marrow, while avoiding out-of-range toxicity.
Once they engraft, the stem cells asymmetrically divide to reproduce themselves, and produce cells which differentiate into many different cell types – including T cells, B cells and monocytes, each of which is expected to carry the therapeutic gene.
Personalized conditioning with Busulfan potentially enables engraftment in the body and brain
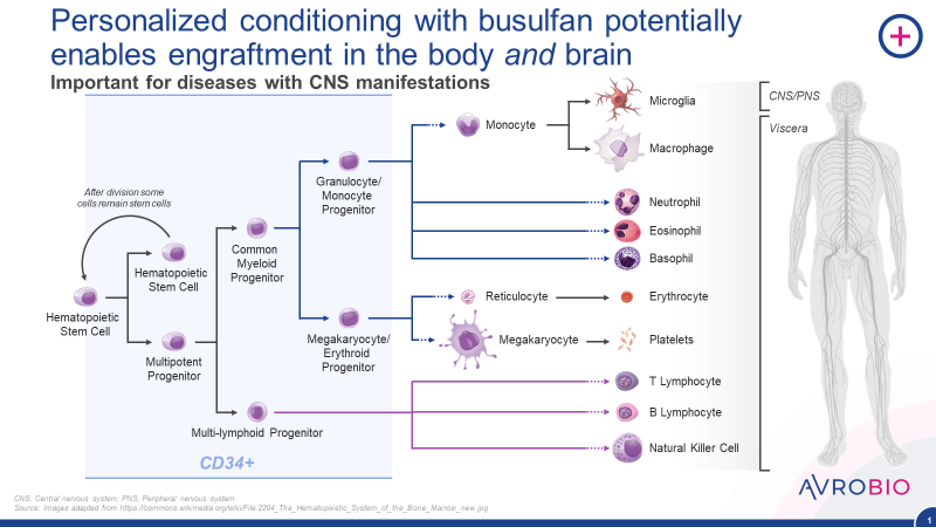
When monocytes enter tissues they become macrophages and in the central nervous system (CNS) they become microglia. The development of monocytes, macrophages and microglia potentially carrying the therapeutic gene could be a crucial differentiator for lentiviral gene therapies. These types of cells are able to traverse the blood-brain barrier and enter the CNS. There, they are expected to engraft and reconstitute a network of microglial-like cells, with each cell expected to be capable of expressing the active protein needed to restore healthy cellular function. Spread out throughout the brain and CNS, these therapeutic cells may be able to slow, halt or even prevent disease progression in the CNS.
Meanwhile, other daughter cells from the original treated batch are expected to continue populating the bone marrow compartments and circulating through the rest of the body, potentially expressing the active protein and distributing it to tissues from heart to muscle to bone.
This is quite a remarkable sequence of events and it speaks to the power of lentiviral gene therapy. At AVROBIO, we believe this modality is ideally suited to any disease that affects the entire body, both systemically and in the brain — which is why we chose the lentiviral vectors for our investigational gene therapies in lysosomal disorders. These relentlessly progressive disorders affect the entire body and can lead to complications in the CNS, as well. To cite just one example, people living with Fabry disease often experience what they refer to as “Fabry fog,” a blurring of cognitive abilities. They are also at an increased risk of recurrent strokes and transient ischemic attacks. We hope our investigational gene therapy will be able to address those complications as well as other systemic complications such as kidney and cardiac disease.
We also hope to be able to use our platform to address diseases in which CNS manifestations are the primary symptoms. Just this month, we announced a new program in Hunter syndrome, a rare and often lethal lysosomal disorder that primarily affects young males. We believe a lentiviral gene therapy approach is well suited to treat this progressive and pervasive disease, which affects organs throughout the body and severely impairs cognitive function.
We hope to be able to use lentiviral gene therapy to treat even very young patients, reaching them before their symptoms develop and irreversible damage occurs. That’s the goal of our Hunter syndrome program, which we expect to enter the clinic next year. The prospect of making such a significant difference to families grappling with devastating disorders is one of the most rewarding aspects of working in lentiviral gene therapy.
Multiple paths to improving patients’ lives
Returning to our discussion at Meeting on the Mesa, I think it was clear to anyone listening that all of our companies are working on exciting and cutting-edge investigational therapies that hold great promise for patients and families. We believe each company has chosen a different delivery system for sound reasons.
At AVROBIO, my colleagues and I are firmly committed to building on lentiviral gene therapy’s proven record and broad utility by continually seeking out new ways we believe we can optimize the technology and improve outcomes for patients. But given the multitude and complexity of genetic diseases, we know it will take many different approaches, advanced by many different companies, to reach the patients with all the different genetic diseases in need. That’s an outcome we can all cheer.